What are the two main types of pain?

What are the two main types of pain? Pain originates in the presence of a noxious stimulus.
That causes an immediate alarm reaction in the person, and our body must preserve it because it is fundamental to the maintenance of life.
https://www.instagram.com/p/CCuwzKYCw0S/
In this article, I want to explain the different types of pain.
Apart from all the classifications of pain treaties, there are two types:
- Neuropathic pain. In this type of affliction, the neurons that encode the suffering are not in good condition.
- Nociceptive pain. It is a suffering that makes sense, the pain that obeys damage, and has a logic.
Neuropathic Pain
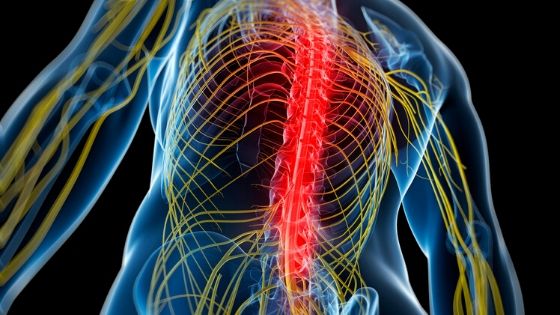
Neuropathic pain is a type of pain that does not initially manifest itself by an injury such as a blow or fracture.
Our own central or peripheral nervous system generates it. It is a type of pain that arises as a direct consequence of an injury or disease that affects our Somatosensory System.
Neuropathic is a torment caused by a malfunctioning of our nervous system. It confuses stimuli such as temperature or touch with painful stimuli.
We can classify Neuropathic pain according to the location of the injury or disease causing the pain:
Peripheral or central
Peripheral or central pain appears as spontaneous discomfort without detectable stimulation. It also appears continuously, regularly, and persistently over time.
Patients, when talking about their pain, usually refer to this type of sensation as:
- Electrical discharge, like a burst of current.
- It was burning, like burning heat.
- Cold tingling.
- Itching or stinging.
- A numb sleeping area.
- A prickly, stinging sensation.
- Tightness
Localized neuropathic pain
Neuropathic pain affects 7-10% of the European population, and 60% of cases are in a specific area of our body. This type of pain is known as Localized Neuropathic.
Chronic neuropathic pain
Chronic is not necessary. For example, I had my tooth removed, three months go by, and it still hurts. That pain is useless.
In the neuropathic, the communication of these neurons is altered, amplified, and altered, and it is already aberrant. They can communicate with other neurons that deal with emotions.
In this neuropathic pain, I already have depression because people sensitive to body suffering are also susceptible to emotions.
Allodynia
Allodynia means that a stimulus that usually doesn't hurt will hurt us. For example, the stimulus of soft-touch does not hurt, but if I come from the beach and get burned, it hurts.
Hyperalgesia
Hyperalgesia is when a stimulus that usually hurts us much more. For example, if I give you a pinch, we all know it hurts, but because of Hyperalgesia, it hurts more.
Neuropathic suffering is difficult to recognize due to its diversity of causes, symptoms, and underlying mechanisms.
That is the reason or reason why it is said to be under-diagnosed. That results in significant reductions in patients' quality of life in the long term.
Nociceptive Pain
Nociceptive agony corresponds to and goes through the standard rational mechanisms of the pain nerve pathways. There is no aberration between the communication of neurons.
Nociceptive pain is a discomfort that we feel as a consequence of an injury, a blow, or other inflammatory processes.
It is the most common one. We can suffer from it, for example:
- When we twist our ankle.
- We experience a burn.
- We hit a finger, among others.
Intense pain senses that we can usually control if we remove the cause of the irritation or treat it medically.
It can also occur when a disease such as arthritis causes it. This condition usually responds to conventional painkillers.
How Nociceptors Work
In response to a noxious stimulus, whether chemical, thermal pressure, or any other characteristic that can cause pain, some free nerve endings called nociceptors.
These will act as receptors of this current information and transmit it to the central nervous system through nerve fibers of type A-delta and C.
In the cellular membrane of these neurons, some receptors can be
- Ionic channels, that is, they modify the transit of ions inside and outside the neuron.
- Metabotropic receptors, i.e., they cause changes in the synthesis of plasma proteins that encode information related to temperature pressure changes.
Propagation of pain by Nociceptors

Once nociceptors are stimulated, they will cause changes in the electrical charge of the neuronal membrane. That will result in the spread of the nerve stimulus to the "dorsal horn" of the spine.
Glutamate release
Glutamate is released, an excitatory amino acid that will bind to a receptor located on a post-synaptic neuron.
This neuron will transmit the information to the central nervous system's higher centers reaching the thalamus and the cerebral cortex.
From these same upper nuclei, downward pathways are set in motion to reach the "dorsal horn" of the spine again.
Release of endogenous substances
They will release endogenous inhibitory substances that will act by modulating the transmission of the stimulus, that is, the amount of information that will be
transmitted from the spinal cord to the higher centers.
Inflammatory response
When the harmful signal is sufficiently intense or long-lasting, a series of mechanisms are triggered to preserve and defend the organism from this external aggression, the so-called "inflammatory response."
When the organism receives signals of external aggression, an infection, a trauma, or an injury, the activate cells related to the inflammatory process as:
These will migrate to the area of injury, causing the release of pro-inflammatory substances such as:
Release of arachidonic acid
These cytokines interact with the enzyme phospholipase, activating it and thus initiating the release sequence of arachidonic acid.
The essential inflammation-related response occurs with the activation of the so-called arachidonic acid cascade.
Arachidonic acid is a constituent element of the cell membrane of all cells in the human body.
When activation of the immune system occurs, the cell membrane releases this acid. When it is free in the cytoplasm, enzymes called cyclooxygenase to attack it.
Bonding of arachidonic acid with cyclooxygenases
As arachidonic acid binds to these cyclooxygenases, they will change their chemical structure.
That will lead to the formation of a large family of substances called Eicosanoids. There are three families:
The prostaglandins, released in response to this activation, cause a generalized inflammatory response.
This response affects different systems in the body:
- The cardiovascular system.
- Musculature.
- Immune system.
- Autonomous system.
They will cause the typical response of hyperthermia, edema, and pain that the Romans already knew:
- Heat.
- Flushing.
- Tumor.
- Pain.
Chronic pain
Sometimes inflammation becomes a pathological process. In this case, chronic suffering has lost its defense function to become an entity that does not contribute anything to the healing process.
Usually, on the contrary, it is a brake that worsens the quality of life and increases the patient's suffering.
Since 1992, we know at least two forms of the cyclooxygenase enzyme have, namely, cox-1 and cox-2. Both participate in the regulation of homeostasis with relatively evenly distributed roles.
Cox-1
Cox-1 is responsible for the synthesis of prostaglandins, which are determinants of cardiovascular function. Mainly antiplatelet antithrombotic and in the intestinal tissue.
Cox-2
The cox-2 is involved in functions related to:
- Myostasis in the kidney.
- The central nervous system.
- The vascular endothelium.
- Stomach.
- The prostate and the ovaries.
It also plays a critical role in the pain response as has been found to overexpress itself by increasing its expression up to 20 times.
Where does the pain occur?
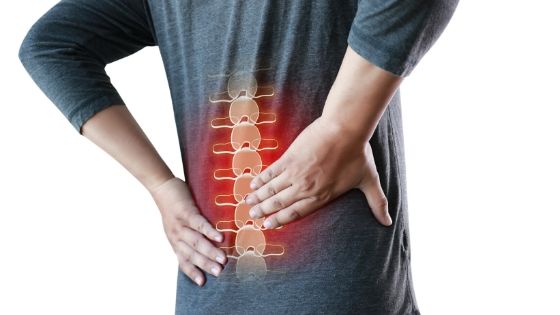
We know that pain is a universal human experience. We now know that pain is produced 100% in the brain. That includes all types of pain, no matter how sharp, dull, strong, or soft it feels, and no matter how long it lasts.
Acute pain
We can feel it for weeks or months is acute pain and is common in:
- Tissue injuries.
- Back problems.
- Ankle sprains.
They will usually encourage you to stay active and gradually return to your activities, including work.
Chronic pain
If you've had this suffering for three months or more, it's called persistent or chronic.
You can find more information about our body or how to be healthy in our health section.

